Fifth year results from a UK study shows that bowel cancer screening halved emergency hospital admissions due to the disease and significantly cut death rates in Coventry and North Warwickshire, one of the UK's first pilot sites. The study is the work of Steve Goodyear, Clinical Sciences Research Institute, University Hospitals Coventry and Warwickshire NHS Trust, Coventry, and colleagues, and will be published online ahead of print in the BMJ journal Gut in the next few days. The scope of the study covers Coventry and Warwickshire in the Midlands, the only UK region to pilot the feasibility of using a home screening kit to collect and post fecal occult blood test samples from subjects aged 50 to 69. A fecal occult blood test looks for blood in the stool, a prime indicator of cancerous and pre-cancerous changes in the gut. Bowel cancer is the second leading cause of cancer deaths in the UK, where it kills more than 16,000 people a year and estimates from Cancer Research UK show one in 20 people is likely to get it. 187,777 individuals aged 50-69 years, who were registered with a general practitioner (GP) in the Coventry and Warwickshire region were asked to collect and post stool samples twice a year using a home screening kit. The study has recently finished its third round of screening in advance of the roll out at national level. Nearly 57 per cent of invited participants completed the first round of screening tests. Those whose results tested positive (1.9 per cent) were invited to a pre-assessment for colonoscopy. In the first 2 years of the study, about 1,700 colonoscopies were carried out as a result of a positive fecal occult blood test from the home kit. In the first round, the overall detection rate for colorectal cancer was 1.62 per 1,000 screening colonoscopies. Figures for the second round were comparable, uptake was 52 per cent, positive tests were found 1.8 per cent of 127,746 participants, around 1,000 screening colonoscopies were performed, with an overall colorectal cancer detection rate of 0.94 per 1000. The researchers also traced the emergency admissions and deaths within 30 days due to bowel cancer between 1999 and 2004 in the largest Midlands hospital trust that serves the region where the pilot screening was being carried out. In that time 1,236 new bowel cancer cases were diagnosed, or around 200 a year. This is in line with national incidence rates, as estimated by Cancer Research UK, said the researchers. The figures showed that in 1999, a year before the postal testing system was introduced, nearly 30 per cent of bowel cancer patients had to be admitted to hospital as an emergency case. But by 2004, this figure had dropped to just under 16 per cent. This drop in emergency bowel cancer cases led to a 50 per cent reduction in emergency operations and a fall in deaths within 30 days from 48 per cent in 1999 to 13 per cent in 2004. The number of stage 3 or Dukes C (relatively advanced) bowel cancers also went down from 38 in 1999 to 16 in 2004, although the same proportion still required emergency care, said the researchers. The researchers concluded that while bowel cancer screening was proved to be effective, the take up rate of the home kit test by those who should be screened regularly appears to be falling. They also warned that by reducing the target group to those aged between 60 and 69 (the pilot covered 50 to 69), the national plan when rolled out may not be as effective as people might hope. All patients and family doctors should be aware of the benefits of screening said the authors. See Full Article
 A 55 year old nurse from Thornton Heath, Surrey was suspended on Friday, 23 November, 2007 at a Conduct and Competence hearing of the Nursing and Midwifery Council in London. Mr. Tennyon Lansana was employed by Bromley Hospital NHS Trust at the Princess Royal University Hospital in Farnborough, Kent when on several occasions he demonstrated a lack of standards of knowledge, skill and judgment required to practice without supervision as a staff nurse on a medical ward. Following a two day hearing, an independent panel of the Nursing and Midwifery Council's (NMC) Conduct and Competence Committee found that his fitness to practice was impaired and that he should be suspended from the Register for a period of 1 year. During this time he may undertake further training and education in order to bring his level of competence up to the standard expected of any nurse working in the UK. Commenting on the outcome of the hearing, NMC spokesperson Leila Harris said, "The panel reached this decision having heard the evidence that proved the charge before it. Mr. Lansana did not possess the requisite knowledge, skills and abilities for lawful, safe and effective practice without direct supervision as set out in the NMC Code of Conduct. The panel has a duty to act in the public interest and to preserve the public's confidence in the profession." The Nursing and Midwifery Council (NMC) is the UK regulator for two professions, nursing and midwifery. The primary purpose of the NMC is protection of the public. It does this through maintaining a register of all nurses, midwives and specialist community public health nurses eligible to practice within the UK and by setting standards for their education, training and conduct. Currently the number of registrants exceeds 682,000. The Nursing and Midwifery Order 2001 (The Order), sets out the NMC's role and responsibilities. The independent panel is selected from a pool of individuals appointed by the Appointments Board. They come from a variety of backgrounds and are not NMC Council members, nor do they sit on any committee of the Council. See Full Article
 New research funded by the MS Society has shown that Botox injections to the bladder provide benefits for people with multiple sclerosis (MS) with sustained improvements to their overall quality of life. Bladder problems are a common and disabling symptom of MS where both storage and emptying processes can be disrupted. Incontinence is common and being unable to 'hold on' (known as urgency) is understandably considered by many people with MS to be one of the most troubling symptoms they face. In the recent research, carried out at the National Hospital for Neurology and Neurosurgery, 43 people with MS who had severe incontinence problems were treated with botulinum neurotoxin type A (Botox) bladder muscle injections. The action of the injection on the bladder is complex but its overall effect is to reduce involuntary contractions and so reduce frequency of urination and urgency. The £200,000 study showed significant improvements in incontinence episodes and the frequency of urination both day and night. There were also sustained improvements in all quality of life measures used and frequency of urination returned to near normal. Dr. Laura Bell, Research Communications Officer for the MS Society, said: "Living with symptoms such as bladder problems can be extremely distressing and restrictive, but this type of treatment can make a tangible and substantial improvement to people's lives and we hope it will become part of standard care for people with MS who need it." The typical duration of the effect of the treatment was 10 months and similar results were seen with repeat treatments. This treatment is not yet licensed in the UK and is consequently not yet widely available for people with MS. Professor Clare Fowler, Consultant in Uro-Neurology at The National Hospital for Neurology and Neurosurgery said: "This study was done as part of a research investigation and the treatment is not widely available. This is because bladder injections of Botox have not yet been licensed and although studies by the pharmaceutical company are ongoing it will probably take a few more years. "This research has been extremely valuable in establishing a clinical method, researching why the treatment works so very well, and providing an opportunity to demonstrate the minimally invasive injection technique to more than 60 visitors, mostly UK consultant urologists, who attended as observers." See Full Article
A vaccine used to protect travelers from cholera, an infection characterized by diarrhea and severe dehydration, could also be used effectively among those living in cholera-prone (endemic) areas, according to a research study by Ira Longini and colleagues published in PLoS Medicine. The study lends support to the idea that public-health officials should consider mass vaccination in their efforts to control endemic cholera. Using a mathematical model for cholera transmission based on information from the Matlab region of Bangladesh, the researchers predicted that cholera outbreaks could be controlled by vaccinating as few as half of the population in an affected region. Because of "herd immunity" - protection of unvaccinated individuals due to the inability of cholera bacteria (Vibrio cholerae) to reach them via their vaccinated neighbors - the model indicated that vaccinating only 50% of the population could reduce the number of cholera cases among unvaccinated people by 89% and among the entire population by 93%. With only a third of the population vaccinated, the number of cases of cholera would still be predicted to fall by three-quarters. In areas where there is less natural immunity to cholera - many people in Matlab are constantly exposed to V. cholerae, so they develop some immunity even without vaccination - 70% of the population would probably need to be vaccinated to control cholera, according to the model. The best way to prevent cholera, which is believed to cause about 100,000 deaths per year in developing countries, is to ensure that everyone has access to safe water and good sanitation, but these remain unavailable in many countries, and in situations of population displacement such as refugee camps and disasters such as floods. The research is discussed in a related perspective article by Lorenz von Seidlein. See Full Article
Researched by Anthony
SADS, or sudden arrhythmia death syndrome, is a term used to describe sudden death due to cardiac arrest brought on by an arrhythmia. The most common cause of sudden death in the US is coronary artery disease. Approximately 300,000 people die suddenly of this cause every year in the US. SADS can also occur from other causes. Also, there are many inherited conditions and heart diseases that can affect young people that can cause sudden death. Many of these victims have no symptoms before dying suddenly. Causes of SADS in young people are long QT syndrome, Brugada syndrome, Catecholaminergic polymorphic ventricular tachycardia and hypertrophic cardiomyopathy and arrhythmogenic right ventricular dysplasia ("arrythmia"-causing, "right ventricle"-involving, pre-cancerous malformation). Referencehttp://www.wikipedia.org
Researched by Anthony Cardiac arrhythmia Cardiac arrhythmia is any of a group of conditions in which the electrical activity of the heart is irregular or is faster or slower than normal. Some arrhythmias are life-threatening medical emergencies that can cause cardiac arrest and sudden death (see SADS). Others cause aggravating symptoms, such as an awareness of a different heart beat, or palpitation, which can be annoying. Some are quite minor and can be regarded as normal. Sinus arrhythmia is the mild acceleration followed by slowing of the normal rhythm that occurs with breathing. In adults the normal resting heart rate ranges from 60 beats per minute to 100 beats per minute. The normal heart beat is controlled by a small area in the upper chamber of the heart called the sinoatrial node or sinus node. The sinus node contains specialized cells that have spontaneous electrical activity that starts each normal heart beat. Faster and slower arrhythmiasIn an adult, a heart rate faster than 100 beats/minute is considered tachycardia. This number varies with age, as the heartbeat of a younger person is naturally faster than that of an older person's. During exercise the sinus node increases its rate of electrical activity to accelerate the heart rate. Such normal fast rate that develops is called sinus tachycardia. In contrast, arrhythmias that are due to fast, abnormal electrical activity can cause tachycardias that are dangerous. If the ventricles of the heart experience one of these tachycardias for a long period of time, there can be deleterious effects. Individuals may sense a tachycardia as a pounding sensation of the heart, known as palpitations. If a tachycardia lowers blood pressure it may cause lightheadedness or dizziness, or even fainting (syncope). If the tachycardia is too fast, the pump function of the heart is impeded, and rarely may lead to sudden death. Most tachycardias are not dangerous. Anything that increases adrenaline or its effects on the heart will increase the heart rate and potentially cause palpitations or tachycardias. Causes include stress, ingested or injected substances (ie: caffeine, amphetamines, alcohol), and an overactive thyroid gland (hyperthyroidism). Individuals who have a tachycardia are often advised to limit or remove exposure to any causative agent. However, these causative agents are not the only contributors to tachycardias and their prevalence has not been evaluated statistically. A slow rhythm, known as bradycardia (less than 60 beats/min), is usually not life threatening, but may cause symptoms. It may be caused by reversible causes (low oxygen, electrolyte abnormalities), or be more permanent (heart block). When it causes symptoms implantation of a permanent pacemaker may be needed. Either dysrhythmia requires medical attention to evaluate the risks associated with the arrhythmia. FibrillationA serious variety of arrhythmia is known as fibrillation. The muscle cells of the heart normally function together, creating a single contraction when stimulated. Fibrillation occurs when the heart muscle begins a quivering motion due to a disunity in contractile cell function. Fibrillation can affect the atrium (atrial fibrillation) or the ventricle (ventricular fibrillation); ventricular fibrillation is imminently life-threatening. Atrial fibrillation is the quivering, chaotic motion in the upper chambers of the heart, known as the atria. Atrial fibrillation is often due to serious underlying medical conditions, and should be evaluated by a physician. It is not typically a medical emergency. Ventricular fibrillation occurs in the ventricles (lower chambers) of the heart; it is always a medical emergency. If left untreated, ventricular fibrillation (VF, or V-fib) can lead to death within minutes. When a heart goes into V-fib, effective pumping of the blood stops. V-fib is considered a form of cardiac arrest, and an individual suffering from it will not survive unless cardiopulmonary resuscitation (CPR) and defibrillation are provided immediately. CPR can prolong the survival of the brain in the lack of a normal pulse, but defibrillation is the intervention which is most likely to restore a more healthy heart rhythm. It does this by applying an electric shock to the heart, after which sometimes the heart will revert to a rhythm that can once again pump blood. Almost every person goes into ventricular fibrillation in the last few minutes of life as the heart muscle reacts to diminished oxygen or general blood flow, trauma, irritants, or depression of electrical impulses themselves from the brain. Origin of impulseWhen an electrical impulse begins in any part of the heart, it will spread throughout the myocardium and cause a contraction. Abnormal impulses can begin by one of two mechanisms: automaticity or reentry. AutomaticityAutomaticity refers to a cardiac muscle cell firing off an impulse on its own. Every cardiac cell has this potential: if it does not receive any impulses from elsewhere, its internal "pacemaker" will fire off an impulse after a certain amount of time. A single specialized location in the atrium, the sinoatrial node, has a higher automaticity (a faster pacemaker) than the rest of the heart, and therefore is usually the one to start the heartbeat. Any part of the heart that initiates an impulse without waiting for the sinoatrial node is called an ectopic focus, and is by definition a pathological phenomenon. This may cause a single premature beat now and then, or, if the ectopic focus fires more often than the sinoatrial node, it can produce a sustained abnormal rhythm. Rhythms produced by an ectopic focus in the atria, or by the atrioventricular node, are the least dangerous dysrhythmias; but they can still produce a decrease in the heart's pumping efficiency, because the signal reaches the various parts of the heart muscle with slightly different timing than usual and causes a poorly coordinated contraction. Conditions that increase automaticity include sympathetic nervous system stimulation and hypoxia. The resulting heart rhythm depends on where the first signal begins: if it is the sinoatrial node, the rhythm remains normal but rapid; if it is an ectopic focus, many types of dysrhythmia can result. Re-entryRe-entry dysrhythmias occur when an electrical impulse travels in a circle within the heart, rather than moving outward and then stopping. Every cardiac cell is able to transmit impulses in every direction, but will only do so once within a short period of time. Normally the impulse spreads through the heart quickly enough that each cell will only respond once, but if conduction is abnormally slow in some areas, part of the impulse will arrive late and will be treated as a new impulse, which can then spread backward. Depending on the timing, this can produce a sustained abnormal rhythm, such as atrial flutter, a self-limiting burst of supraventricular tachycardia, or the dangerous ventricular tachycardia. By analogy, imagine a room full of people all given these instructions: "If you see anyone starting to stand up, then stand up for three seconds and sit back down." If the people are quick enough to respond, the first person to stand will trigger a single wave which will then die out; but if there are stragglers on one side of the room, people who have already sat down will see them and start a second wave, and so on. DiagnosisCardiac dysrhythmias are often first detected by simple but nonspecific means: auscultation of the heartbeat with a stethoscope, or feeling for peripheral pulses. These cannot usually diagnose specific dysrhythmias, but can give a general indication of the heart rate and whether it is regular or irregular. Not all the electrical impulses of the heart produce audible or palpable beats; in many cardiac arrhythmias, the premature or abnormal beats do not produce an effective pumping action and are experienced as "skipped" beats. The simplest specific diagnostic test for assessment of heart rhythm is the electrocardiogram (abbreviated ECG or EKG). A Holter monitor is an EKG recorded over a 24-hour period, to detect dysrhythmias that may happen briefly and unpredictably throughout the day. List of common cardiac arrhythmias* Atrial Rhythms o Premature Atrial Contractions (PACs) o Wandering Atrial Pacemaker o Multifocal atrial tachycardia o Supraventricular tachycardia (SVT) o Atrial flutter o Atrial fibrillation (Afib) * Ventricular Rhythms o Premature Ventricular Contractions (PVC) o Accelerated idioventricular rhythm o Ventricular tachycardia o Ventricular fibrillation o Polymorphic ventricular tachycardia * Atrial Ventricular Arrythmias o AV nodal reentrant tachycardia o AV reentrant tachycardia · + Wolff-Parkinson-White syndrome · + Lown-Ganong-Levine syndrome * Junctional Arrhythmias o Junctional rhythm o Junctional tachycardia o Premature junctional complex * Heart Blocks, also known as AV blocks o First degree heart block, also known as PR prolongation o Second degree heart block · + Type 1 Second degree heart block, also known as Mobitz I or Wenckebach · + Type 2 Second degree heart block, also known as Mobitz II o Third degree heart block, also known as complete heart block Less common arrhythmiasTrigeminal rhythm (or trigeminy) is a kind of arrhythmia where hearbeats occur in groups of threes. These three beats are usually one beat from the SA node, followed by two extrasystolic beats. It is a possible cardiovascular side effect of SSRI treatment. Antiarrhythmic therapiesThere are many classes of antiarrhythmic medications and many individual drugs within these classes. Dysrhythmias may also be treated electrically. Cardioversion is the application of electrical current across the chest wall to the heart and it is used for treatment of supraventricular or pulsed ventricular tachycardia. Defibrillation differs in that it is used for ventricular fibrillation and pulseless ventricular tachycardia, and more electricity is delivered with defibrillation than with cardioversion. In cardioversion, the recipient is either sedated or lightly anesthetized for the procedure. In defibrillation, the recipient has lost consciousness so there is no need for sedation. Electrical treatment of dysrhythmia includes cardiac pacing. Temporary pacing may be done for very slow heartbeats, or bradycardia, from drug overdose or myocardial infarction. A pacemaker may be placed in situations where the bradycardia is not expected to recover. Atrial fibrillation can also be treated through a procedure, e.g. pulmonary vein isolation. This is performed by a cardiologist who specializes in electrophysiology and is done percutaneously with catheters. Alternatively, a maze procedure can be performed through cardiothoracic surgery. Fatty acidsFatty acids play an important role in the life and death of cardiac cells because they are essential fuels for mechanical and electrical activities of the heart. Referencehttp://www.wikipedia.orgIf you find an error, please let us know.
SVD in medicine stands for Spontaneous Vaginal Delivery, which is also known as Normal Spontaneous Vaginal Delivery, Vaginal Birth, and Normal Vaginal Delivery. See Additional Information
 A breakthrough in stem cell research was announced last week in a paper in the journal Science where researchers from the University of Wisconsin -Madison in the US and other colleagues reported how they reprogrammed human skin cells to behave like embryonic stem cells. The report is grabbing the headlines not just because of the remarkably simple elegance of the science, the fact that introducing four genes is all that is needed to "reprogram human somatic cells to pluripotent stem cells that exhibit the essential characteristics of embryonic stem cells", but also because of the profound impact it appears to be having on the ethical debate surrounding stem cell research. Leading bioethicists like R. Alta Charo, a UW-Madison professor of law and bioethics are saying that the discovery is starting to "redefine the political and ethical dynamics of the stem-cell debate", and could neatly sidestep the ethical and legal problems surrounding use of embryonic stem cells, because, as Charo explained: "This is a method for creating a stem cell line without ever having to work through, at any stage, an entity that is a viable embryo." The research was carried out in the lab of UW-Madison biologist and professor of anatomy at the University of Wisconsin School of Medicine and Public Health, James Thomson, the scientist who in 1998 was the first to recover embryonic stem cells from human embryos. This time the study was led by Junying Yu of the Genome Center of Wisconsin and the Wisconsin National Primate Research Center. Speaking about this latest breakthrough, Thomson said: "The induced cells do all the things embryonic stem cells do. It's going to completely change the field." Embryonic stem cells are valued above all others because so far they are the only kind shown to be truly "pluripotent", that is having the capacity to become any of the 220 types of cell in the human body. They have the potential to generate new heart, liver, brain, muscle and bone tissue, and replace diseased or damaged tissue in people who are ill with cardiovascular, Alzheimer's, Parkinson's and a whole range of the other diseases including diabetes. Scientists at UW-Madison said that the new method developed by Yu and colleagues brings the generation of pluripotent stem cells within easy reach of many labs of "moderate sophistication". The other advantage of the new method is the fact that using cells drawn from the patient's own skin, the stem cells can be customized to the patient, bringing numerous benefits, such as the elimination of immune system rejection. See Full Article
Compiled and Summarized by Alex Normal Spontaneous Vaginal Delivery a.k.a. Vaginal Birth, Spontaneous Vaginal Delivery, Normal Vaginal Delivery, is the term used to describe any delivery of the baby through the vagina (versus a c-section delivery). The baby typically comes through head first. If the baby is not head first, (e.g., breech) it may need to be delivered by c-section. VariationsWhen the amniotic sac has not ruptured during labor or pushing, the infant can be born with the membranes intact. This is referred to as "being born in the caul." The caul is harmless and easily wiped away by the doctor or person assisting with the childbirth. In medieval times, a caul was seen as a sign of good fortune for the baby, in some cultures was seen as protection against drowning, and the caul was often impressed onto paper and stored away as an heirloom for the child. With the advent of modern interventive obstetrics, premature artificial rupture of the membranes has become common and it is rare for infants to be born in the caul in Western births. Pain controlDue to the relatively-large size of the human skull and the shape of the human pelvis forced by the erect posture, childbirth is more difficult and painful for human mothers than other mammals. Many methods are available to reduce the pain of labor, including psychological preparation, emotional support, epidural analgesia, spinal anesthesia, nitrous oxide and opioids, the Lamaze Technique. Each method has its own advantages and disadvantages. ComplicationsComplications occasionally arise during childbirth; these generally require management by an obstetrician. Non-progression of labor (longterm contractions without adequate cervical dilation) is generally treated with cervical prostaglandin gel or intravenous synthetic oxytocin preparations. If this is ineffective, Caesarean section may be necessary. Fetal distress is the development of signs of distress by the child. These may include rising or decreasing heartbeat (monitored on cardiotocography/CTG), shedding of meconium in the amniotic fluid, and other signs. Non-progression of expulsion (the head or presenting parts are not delivered despite adequate contractions): this can require interventions such as vacuum extraction, forceps extraction and Caesarian section. In the past, a great many women died during or shortly after childbirth but modern medical techniques available in industrialized countries have greatly reduced this total. Social aspectsIn modern times, participation of the father during childbirth is now the norm. However, before the 1960's, in most cultures the father was forbidden to enter childbirth area, as were other men with the exception of the doctor. The exception to this rule were Poleshuks from Polesie. In this culture the wife gave birth sitting on her husband's knees. Legal aspectsIn many legal systems, the place of childbirth decides nationality of a child. The birth certificate is the basic document, which proves that the individual is a human being. Referenceshttp://www.doctorslounge.comServed as primary source. http://pennhealth.comServed as reference.
The research team from the Department of Electronics and Computer Science at the University of Granada (UGR), together with the Department of Radiology at the Hospital Virgen de las Nieves in Granada, have designed a portable and low-cost device which can measure the ionizing radiation someone is exposed to, for example, during radiotherapy. Ionizing radiations play a vital role in the treatment and diagnosis of malignant neoplastic illnesses as well as in the diagnosis of other pathologies. However, according to Manuel Vilches Pacheco from the Medical Physics and Radiology Department at the Hospital Virgen de las Nieves in Granada, "the potential harm ionizing radiations can cause means that, in order to obtain clinical benefits and reduce the onset of unwanted adverse effects as much as possible, they must be used under strict quality control." According to experts, this is why it is important to develop instruments which can verify the final result by carrying out a direct follow-up of treatments administered to patients, such as image registration (portal imaging system) or the in vivo measurement of the exact dose administered to patients. See Full Article
Description: Normal Vaginal Delivery of a baby Note: You need the latest Flash Player in order to view the video. Download it here. You may see an alternative video demonstration on this site: Normal Spontaneous Vaginal DeliveryNSVD (Normal Spontaneous Vaginal Delivery), also called Vaginal Birth, Normal Vaginal Delivery, or Spontaneous Vaginal Delivery, is a method of delivering the baby the natural way, or through the vagina. The procedure varies from country to country, or per institution or hospital so we cannot give the overall procedure. However, we will give some of the most important tips to consider. This may also serve as an insight as to what's really going on in an actual event. See additional info
A US study has found that the cortex area of the brain is thicker in people who have migraines compared to those who do not. The researchers do not know whether the difference causes the migraine or having migraine over the years has led to the difference in brain structure. The study is published in the 20th November online issue of the journal Neurology and is the work of Dr. Nouchine Hadjikhani, of The Martinos Center for Biomedical Imaging at Massachusetts General Hospital in Charlestown, Massachusetts, and colleagues. Dr. Hadjikhani and colleagues compared 24 people who suffered from migraine with 12 people who did not, and found that the somatosensory cortex (SSC) area of the brain of those with migraine was on average 21 percent thicker. "Repeated migraine attacks may lead to, or be the result of, these structural changes in the brain," said Hadjikhani in a prepared statement. "Most of these people had been suffering from migraines since childhood, so the long-term overstimulation of the sensory fields in the cortex could explain these changes," she added. Alternatively, the researchers suggested it could be that people who develop migraines are naturally more sensitive to stimulation. Using magnetic resonance imaging (MRI), the researchers had already discovered there were structural differences between the brains of people with migraine and people without. In this new research they measured group and individual differences in cortical thickness in migraine patients who were matched for age and sex with healthy subjects. The results showed that the people who suffered from migraine had on average 21 per cent thicker SSCs than those who did not, and the most significant differences in cortical thickness were in what is known as the caudal (tail) SSC, where sensations from the trigeminal area, the head and face, are processed. Most of the migraine patients had been getting migraines since they were children. This might suggest that long term stimulation of the cortex over such a long period could lead to structural changes, said Hadjikhani. On the other hand, it could also be that their brain's structure changed progressively for some other reason and this led to the headaches. However, regardless of the cause and effect question, the results show that the sensory areas of the brain are important components in migraine. "This may explain why people with migraines often also have other pain disorders such as back pain, jaw pain, and other sensory problems such as allodynia, where the skin becomes so sensitive that even a gentle breeze can be painful," added Hadjikhani. The researchers concluded that the SSC plays a key role in the processing of "noxious and nonnoxious" somatosensory signals, and that: "Thickening in the SSC is in line with diffusional abnormalities observed in the subcortical trigeminal somatosensory pathway of the same migraine cohort in a previous study. Repetitive migraine attacks may lead to, or be the result of, neuroplastic changes in cortical and subcortical structures of the trigeminal somatosensory system." See Full Article
Compiled and Summarized by Alex Uterine fibroids Uterine fibroids are noncancerous growths of the uterus that often appear during childbearing years. Also called fibromyomas, leiomyomas or myomas, uterine fibroids aren't associated with an increased risk of uterine cancer and almost never develop into cancer. As many as three out of four women have uterine fibroids, but most are unaware of them because they often cause no symptoms. The doctor may discover them incidentally during a pelvic exam or prenatal ultrasound. In general, uterine fibroids cause no problems and seldom require treatment. Medical therapy and surgical procedures can shrink or remove fibroids if there is no discomfort or troublesome symptoms. Rarely, fibroids can require emergency treatment if they cause sudden, sharp pelvic pain. Signs and SymptomsUterine fibroids are often asymptomatic. Rapidly enlarging tumors may cause pelvic pain. They are a common cause of heavy or irregular menstrual bleeding. In women of child bearing age, these tumors may produce infertility. Excessive blood loss can lead to signs of anemia, including fatigue, shortness of breath, rapid heart rate and pallor. CausesUterine fibroids develop from the smooth muscular tissue of the uterus (myometrium). A single cell reproduces repeatedly, eventually creating a pale, firm, rubbery mass distinct from neighboring tissue. Fibroids range in size from seedlings, undetectable by the human eye, to bulky masses that can distort and enlarge the uterus. They can be single or multiple, in extreme cases expanding the uterus so much that it reaches the rib cage. Doctors don't know the cause of uterine fibroids, but research and clinical experience point to several factors: · Genetic alterations. Many fibroids contain alterations in genes that code for uterine muscle cells. · Hormones. Estrogen and progesterone, two hormones that stimulate development of the uterine lining in preparation for pregnancy, appear to promote the growth of fibroids. Fibroids contain more estrogen and estrogen receptors than do normal uterine muscle cells. · Other chemicals. Substances that help the body maintain tissues, such as insulin-like growth factor, may affect fibroid growth. DiagnosisUterine fibroids are frequently found incidentally during a routine pelvic exam. The doctor may feel irregularities in the shape of the uterus through the abdomen, suggesting the presence of fibroids. UltrasoundIf confirmation is needed, the doctor may obtain an ultrasound — a painless exam that uses sound waves to obtain a picture of the uterus — to confirm the diagnosis and to map and measure fibroids. A doctor or technician moves the ultrasound device (transducer) over the abdomen (transabdominal) or places it inside the vagina (transvaginal) to obtain images of the uterus. Transvaginal ultrasound provides more detail because the probe is closer to the uterus. Transabdominal ultrasound visualizes a larger anatomic area. Sometimes, fibroids are discovered during an ultrasound conducted for a different purpose, such as during a prenatal ultrasound. Other imaging testsIf traditional ultrasound doesn't provide enough information, the doctor may order other imaging studies, such as: · Hysterosonography. This ultrasound variation uses sterile saline to expand the uterine cavity, making it easier to obtain interior images of the uterus. This test may be useful if there is heavy menstrual bleeding despite normal results from traditional ultrasound. · Hysterosalpingography. This technique uses a dye to highlight the uterine cavity and fallopian tubes on X-ray images. The doctor may recommend it if infertility is a concern. In addition to revealing fibroids, it can help the doctor determine if the fallopian tubes are open. · Hysteroscopy. The doctor inserts a small, lighted telescope called a hysteroscope through the cervix into the uterus. The tube releases a gas or liquid to expand the uterus, allowing the doctor to examine the walls of the uterus and the openings of the fallopian tubes. A hysteroscopy can be performed in the doctor's office. Imaging techniques that may occasionally be necessary include computerized tomography (CT) and magnetic resonance imaging (MRI). Other testsIf the client is experiencing abnormal vaginal bleeding, the doctor may want to conduct other tests to investigate potential causes. He or she may order a complete blood count (CBC) to determine if there is iron deficiency anemia because of chronic blood loss. The doctor may also order blood tests to rule out bleeding disorders and to determine the levels of reproductive hormones produced by the ovaries. PathogenesisFor complete detail. See link. PathophysiologySmooth-muscle tumors of uterine origin encompass a broad family of neoplasms. The leiomyoma, by far the most common of all the neoplasms, generally is hormone sensitive, with rates of growth semiquantitatively related to estrogen and progesterone receptor levels. Several forms of degenerative change can occur in the leiomyoma. The most common is hyaline degeneration, which is important in that it should not be mistaken for the coagulative tumor cell necrosis seen in leiomyosarcoma. Red degeneration (necrobiosis) is a form of degeneration that occurs characteristically but not exclusively in pregnancy, and the process is often the cause of pain and fever. Several forms of treatment have been used medically in the treatment of leiomyoma. Gonadotropin-releasing hormone analogs or agonists or selective arterial embolization with polyvinylformaldehyde particles may lead to substantial degeneration or infarction of the leiomyoma, respectively. Several variants of leiomyoma, the cellular and symplastic leiomyomas, are important to recognize, as they can be misinterpreted as sarcoma. In addition, there are two unusual growth patterns of leiomyoma that are important to recognize. Both the benign metastasizing leiomyoma and disseminated peritoneal leiomyomatosis are found outside the uterus, and neither is malignant. Recent studies offer insights into their origin and hormonal influences. From a diagnostic and therapeutic point of view, the leiomyosarcoma, while rare, is clinically of great import. Coagulative necrosis, cytologic atypia, and mitotic counts are all important in diagnosing the condition. PreventionAlthough researchers continue to study the causes of fibroid tumors, little scientific advice is available on how to prevent them. Preventing uterine fibroids may not be possible, but you can take comfort in the fact that only a small percentage of these tumors require treatment. TreatmentThere's no single best approach to uterine fibroid treatment. Many treatment options exist. In most cases, the best action to take after discovering fibroids is simply to be aware they are there. Watchful waitingIf you're like most women with uterine fibroids, you have no signs or symptoms. In your case, watchful waiting (expectant management) could be the best course. Fibroids aren't cancerous. They rarely interfere with pregnancy. They usually grow slowly and tend to shrink after menopause when levels of reproductive hormones drop. This is the best treatment option for a large majority of women with uterine fibroids. MedicationsMedications for uterine fibroids target hormones that regulate menstrual cycle, treating symptoms such as heavy menstrual bleeding and pelvic pressure. They don't eliminate fibroids, but may shrink them. Medications include: · Gonadotropin-releasing hormone (Gn-RH) agonists. To trigger a new menstrual cycle, a control center in the brain called the hypothalamus manufactures gonadotropin-releasing hormone (Gn-RH). The substance travels to the pituitary gland, a tiny gland also located at the base of the brain, and sets in motion events that stimulate the ovaries to produce estrogen and progesterone. Medications called Gn-RH agonists (Lupron, Synarel, others) act at the same sites that Gn-RH does. But when taken as therapy, a Gn-RH agonist produces the opposite effect to that of the natural hormone. Estrogen and progesterone levels fall, menstruation stops, fibroids shrink and anemia often improves. · Androgens. The ovaries and the adrenal glands, located above your kidneys, produce androgens, the so-called male hormones. Given as medical therapy, androgens can relieve fibroid symptoms. Danazol, a synthetic drug similar to testosterone, has been shown to shrink fibroid tumors, reduce uterine size, stop menstruation and correct anemia. However, occasional unpleasant side effects such as weight gain, dysphoria (feeling depressed, anxious or uneasy), acne, headaches, unwanted hair growth and a deeper voice, make many women reluctant to take this drug. · Other medications. Oral contraceptives or progestins can help control menstrual bleeding, but they don't reduce fibroid size. Nonsteroidal anti-inflammatory drugs (NSAIDs), which are not hormonal medications, are effective for heavy vaginal bleeding unrelated to fibroids, but they don't reduce bleeding caused by fibroids. HysterectomyThis operation — the removal of the uterus — remains the only proven permanent solution for uterine fibroids. But hysterectomy is major surgery. It ends the ability to bear children, and if elected to have ovaries removed also, it brings on menopause and the question of whether you'll take hormone replacement therapy. MyomectomyIn this surgical procedure, the surgeon removes the fibroids, leaving the uterus in place. If you want to bear children, you might choose this option. With myomectomy, as opposed to a hysterectomy, there is a risk of fibroid recurrence. There are several ways a myomectomy can be done: · Abdominal myomectomy. If having multiple fibroids, very large or very deep fibroids, the doctor may use an open abdominal surgical procedure to remove the fibroids. · Laparoscopic myomectomy. If the fibroids are small and few in number, the client and the doctor may opt for a laparoscopic procedure, which uses slender instruments inserted through small incisions in the abdomen to remove the fibroids from the uterus. The doctor views the abdominal area on a remote monitor via a small camera attached to one of the instruments. · Hysteroscopic myomectomy. This procedure may be an option if the fibroids are contained inside the uterus (submucosal). A long, slender scope (hysteroscope) is passed through the vagina and cervix and into the uterus. The doctor can see and remove the fibroids through the scope. This procedure is best performed by a doctor experienced in this technique. Variations of myomectomy — in which uterine fibroids are destroyed without actually removing them — include: · Myolysis. In this laparoscopic procedure, an electric current destroys the fibroids and shrinks the blood vessels that feed them. · Cryomyolysis. In a procedure similar to myolysis, cryomyolysis uses liquid nitrogen to freeze the fibroids. The safety, effectiveness and associated risk of fibroid recurrence of myolysis and cryomyolysis have yet to be determined. · Endometrial ablation. This treatment, performed with a hysteroscope, uses heat to destroy the lining of the uterus, either ending menstruation or reducing the menstrual flow. Endometrial ablation is effective in stopping abnormal bleeding, but doesn't affect fibroids outside the interior lining of the uterus. Uterine artery embolizationSmall particles injected into the arteries supplying the uterus cut off blood flow to fibroids, causing them to shrink. This technique is proving effective in shrinking fibroids and relieving the symptoms they can cause. Advantages over surgery include: · No incision · Shorter recovery time Complications may occur if the blood supply to the ovaries or other organs is compromised. Focused ultrasound surgeryMRI-guided focused ultrasound surgery (FUS), approved by the Food and Drug Administration in October 2004, is a newer treatment option for women with fibroids. Unlike other fibroid treatment options, FUS is noninvasive and preserves the uterus. This procedure is performed while the client is inside of a specially crafted MRI scanner that allows doctors to visualize the anatomy, and then locate and destroy (ablate) fibroids inside the uterus without making an incision. Focused high-frequency, high-energy sound waves are used to target and destroy the fibroids. A single treatment session is done in an on- and off-again fashion, sometimes spanning several hours. Initial results with this technology are promising, but its long-term effectiveness is not yet known. Notes to consider before decidingBefore making a decision, consider the pros and cons of all available treatment options in relation to your particular situation. Remember, most women don't need any treatment for uterine fibroids. ComplicationsAlthough uterine fibroids usually aren't dangerous, they can cause discomfort and may lead to complications such as anemia from heavy blood loss. In rare instances, fibroid tumors can grow out of the uterus on a stalk-like projection. If the fibroid twists on this stalk, a sudden, sharp, severe pain in the lower abdomen may develop. If so, seeking medical care is strongly recommended. Surgery may be needed. Pregnancy and fibroidsBecause uterine fibroids typically develop during the childbearing years, women with fibroids are often concerned about their chances of a successful pregnancy. Fibroids usually don't interfere with conception and pregnancy, but they can occasionally affect fertility. They may distort or block the fallopian tubes, or interfere with the passage of sperm from the cervix to the fallopian tubes. Submucosal fibroids may prevent implantation and growth of an embryo. Research indicates that pregnant women with fibroids are at slightly increased risk of miscarriage, premature labor and delivery, abnormal fetal position, and separation of the placenta from the uterine wall. But not all studies confirm these associations. Furthermore, complications vary based on the number, size and location of fibroids. Multiple fibroids and large submucosal fibroids that distort the uterine cavity are the type most likely to cause problems. A more common complication of fibroids in pregnancy is localized pain, typically between the first and second trimesters. This is usually easily treated with pain relievers. In most cases, fibroids don't interfere with pregnancy and treatment isn't necessary. It was once believed that fibroids grew faster during pregnancy, but multiple studies suggest otherwise. Most fibroids remain stable in size, although some increase or decrease slightly, usually in the first trimester. If there are fibroids and the patient experienced repeated pregnancy losses, the doctor may recommend removing one or more fibroids to improve the chances of carrying a baby to term, especially if no other causes of miscarriage can be found and the fibroids distort the shape of the uterine cavity. Doctors usually don't remove fibroids in conjunction with a Caesarean section because of the high risk of excessive bleeding. References:http://www.mayoclinic.comServed as primary source. http://www.myelectronicmd.comServed as reference. http://www.ehponline.orgSource for Pathophysiology. If you find an error, please let us know.
South Dakota philanthropist Denny Sanford will donate $20 million for the creation of the Sanford Children's Health Research Center. The gift will serve as the foundation for collaboration between Sanford Health of Sioux Falls, South Dakota and the Burnham Institute for Medical Research headquartered in La Jolla, California. This collaboration will combine world-class scientific talent with state-of-the-art technology to conquer childhood diseases. To achieve this goal, the donation will create the Sanford Children's Health Research Center at the Burnham Institute for Medical Research to be located in La Jolla, California. Likewise, Sanford Health will develop a Sanford Children's Health Research Center facility in Sioux Falls, South Dakota. The collaboration between the two locations will establish the basis of an integrated, world-class, academic pediatric research network. "I have the utmost confidence that this collaboration will promote solutions to some of the most troubling health issues that affect children," said Denny Sanford. "Nothing gives me greater pleasure than to encourage efforts and activities that I know will help children enjoy the gift of good health." "Partnering with my generous friend Denny Sanford and the Sanford Health organization brings significant added strength and stature to the Burnham Institute here in San Diego, to our rapidly growing Lake Nona-Orlando research facility, and to our new Burnham-Santa Barbara research program. We welcome them with open arms," said Malin Burnham, Chairman of Burnham's Board of Trustees. As part of the collaboration, Burnham will recruit a world-class research scientist to serve as Scientific Director for the Sanford Children's Health Research Center in La Jolla, and Burnham will advise Sanford in recruiting talented research scientists to work at Sanford Health in Sioux Falls. In addition, Burnham will dedicate nine senior scientists (faculty) to be supported by approximately 40 scientists and related staff in approximately 25,000 square feet of research and support space in La Jolla. The Sioux Falls location will have at least three senior scientists and up to 20 additional scientists and staff. Burnham and Sanford Health will form an oversight committee made up of members from both organizations in order to direct collaborative efforts between both locations. "The opportunity to collaborate with Sanford Health expands our ability to combine Burnham's world-class laboratory research with a powerful clinical partner dedicated to advancing medicine," said Burnham's President and CEO, John C. Reed, MD, PhD. "Denny Sanford's gift and his commitment to improving child health will enable us to consolidate and expand our present pediatric medical research activities and to make more rapid progress towards solving the unmet medical needs of children. We are honored for the opportunity to work with Mr. Sanford and the Sanford Health organization towards this noble goal." "Once again, we thank Mr. Sanford for his generosity and vision," said Sanford Health Executive Vice President Dave Link. "The collaboration with Burnham will have far-reaching, positive and long-term health impacts on children. Collaborative efforts like this one are crucial to achieving our initiatives as well as our overall research success." Mr. Sanford is chairman of United National Corporation, First PREMIER Bank and Premier BANKCARD, Inc. headquartered in Sioux Falls, South Dakota. He has a longtime, special interest in supporting organizations and groups that focus on the health care needs of children. See Full Article
Researched by Alex An X-ray machine utilizes electromagnetic radiation to produce an image of an object, usually with the purpose of visualizing something located below the object's surface. The machine is made up of an X-ray source or X-ray tube, an x-ray detection system, and positioning hardware to align these two components with the object to be imaged. X-rays are produced by bombarding a surface with high speed electrons (in a vacuum). One of the first X-ray photographs was made of the hand of Röntgen's wife. The image displayed both her wedding ring and bones. How they workAn X-ray imaging system consists of a X-ray source or generator, and an image detection system which can either be comprised of film (analog technology) or a digital capture system. X-ray SourcesIn the typical X-ray source of less than 450 kV, X-ray photons are produced by an electron beam striking a target. The electrons that make up the beam are emitted from a heated cathode filament. The electrons are then focused and accelerated towards an angled anode target. The point where the electron beam strikes the target is called the focal spot. Most of the kinetic energy contained in the electron beam is converted to heat, but around 10% of the energy is converted into X-ray photons, the excess heat is dissipated via a heat sink. At the focal spot, X-ray photons are emitted at 180° from the target surface, the highest intensity being around 60° to 90°, there is a small round window in the X-ray tube directly above the angled target. This window allows the X-ray to exit the tube with little attenuation while maintaining a vacuum seal required for the X-ray tube operation. X-ray machines work by applying controlled voltage, current, and time to the X-ray tube, which results in a beam of X-rays. The beam is projected on matter. Some of the X-ray beam will pass through the object, while some are reflected. The resulting pattern of the radiation is then ultimately detected by a detection medium including rare earth screens (which surround photographic film), semiconductor detectors, or X-ray image intensifiers. X-Ray DetectionIn health care applications in particular, the x-ray detection system rarely consists of the detection medium. For example, a typical stationary radiographic x-ray machine also includes an ion chamber and grid. The ion chamber is basically a hollow plate located between the detection medium and the object being imaged. It determines the level of exposure by measuring the amount of x-rays that have passed through the electrically charged, gas-filled gap inside the plate. This allows for minimization of patient radiation exposure by both ensuring that an image is not underdeveloped to the point the exam needs to be repeated and ensuring that more radiation than needed is not applied. The grid is usually located between the ion chamber and object and consists of several lead slats stacked next to each other (resembling open window blinds). In this manner, the grid allows straight x-rays to pass through to the detection medium but absorbs reflected x-rays. This improves image quality by preventing reflected (non-diagnostic) x-rays from reaching the detection medium allowing for lower exam doses overall. Images taken with such devices are known as X-ray photographs or radiographs. The older term Röentgenogram continues to be used by radiologists. Medical UsesThere are two basic areas in which Health Care uses X-radiation; Radiography, and Dental Hygine. Radiography is used for fast, highly penetrating images. Usually it's used on areas with a high bone content. Some forms of radiography uses are Panoramic X-rays, Radiography, Mammography, Tomography, and Radiotherapy. Fluoroscopy is used in cases where real-time visualization is necessary. You may have seen a type of fluorography at the airport. Some of the uses of Fluorography are Angiography, barium enemas, barium swallows, biopsies, and hip replacement. X-rays are highly penetrating, ionizing radiation, and X-ray machines are used in radiology to take pictures of bones and teeth. This is because bones absorb the radiation more than the less-dense soft tissue. X-rays from a source pass through the body and onto a photographic cassette. Areas where radiation is absorbed show up as lighter shades of gray (closer to white). This can be used to diagnose broken or fractured bones. Imaging of the digestive tract is done with the help of a radiocontrast agent such as barium sulfate, which is opaque to X-rays. Source: WikipediaIf you find an error, please let us know.
Researched by Alex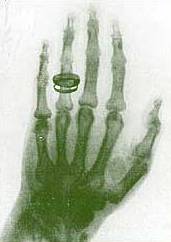 X-rays (or Röntgen rays) are a form of electromagnetic radiation with a wavelength in the range of 10 to 0.01 nanometers, corresponding to frequencies in the range 30 PHz to 30 EHz. X-rays are primarily used for diagnostic radiography and crystallography. X-rays are a form of ionizing radiation and as such can be dangerous. In many languages it is called Röntgen radiation after one of the first investigators of the X-rays, Wilhelm Conrad Röntgen. Units of Measure and ExposureThe rem is the traditional unit of Dose Equivalent. This describes the Energy delivered by γ or X - radiation (indirectly ionizing radiation) for humans. The SI counterpart is the Sievert (Sv). One Sievert is equal to 100 rem. Because the rem is a relatively large unit, typical equivalent Dose is measured in millirem (mrem), or one thousandth of a rem The average person living in the United States is exposed to approximately 150 mrem annually from background sources alone. Reported dosage due to dental X-rays seems to vary significantly. Depending on the source, a typical dental X-ray of a human results in an exposure of perhaps, 3, 40, 300, or as many as 900 mrems. Medical UsesSince Röntgen's discovery that X-rays can identify bony structures, X-rays have been developed for their use in medical imaging. Radiology is a specialized field of medicine. Radiographers employ radiography and other techniques for diagnostic imaging. Indeed, this is probably the most common use of X-ray technology. X-rays are especially useful in the detection of pathology of the skeletal system, but are also useful for detecting some disease processes in soft tissue. Some notable examples are the very common chest X-ray, which can be used to identify lung diseases such as pneumonia, lung cancer or pulmonary edema, and the abdominal X-ray, which can detect ileus (blockage of the intestine), free air (from visceral perforations) and free fluid (in ascites). In some cases, the use of X-rays is debatable, such as gallstones (which are rarely radiopaque) or kidney stones (which are often visible, but not always). Also, traditional plain X-rays pose very little use in the imaging of soft tissues such as the brain or muscle. Imaging alternatives for soft tissues are computed axial tomography (CAT or CT scanning), magnetic resonance imaging (MRI) or ultrasound. Since 2005, X-rays are listed as a carcinogen by the U.S. government. Radiotherapy, a curative medical intervention, now used almost exclusively for cancer, employs higher energies of radiation. The efficiency of X-ray tubes is less than 2%. Most of the energy is used to heat up the anode. Source: http://www.wikipedia.orgIf you find an error, please let us know.
 A new US study suggests that the osteoporosis drug Forteo (made by Eli Lilly) was more effective than Fosamax (made by Merck) at increasing bone density in arthritis patients with osteoporosis caused by taking corticosteroids such as prednisone. The study is the work of Dr. Kenneth Saag, a professor in the Division of Clinical Immunology and Rheumatology at the University of Alabama at Birmingham (UAB) and colleagues, and is published in the 15th November issue of the New England Journal of Medicine. The study showed that patients taking Forteo (teriparatide), a parathyroid hormone, more than doubled their bone density and significantly reduced their risk of new spinal fractures compared to those who took Fosamax (alendronate). A great number of arthritis and other patients use prednisone and other glucocorticoids to lessen inflammation and reduce swelling in tissue and joints. However there is a downside to the drugs, the possibility of bone loss and osteoporosis, a bone disease that results in bones becoming fragile and prone to fracture. Saag said that patients with arthritis need to be on medication for their condition, but it is also important that they reduce the risk of hip fracture or spinal compression from taking their medication, thus "patients and their doctors need more bone-building options," he said. "This study significantly improves our understanding of treatment options for secondary osteoporosis, which is osteoporosis caused by taking glucocorticoid drugs like prednisone," explained Saag. Current international guidelines recommend the class of drugs that includes Fosamax, called bisphosphonates, for the treatment of glucocorticoid-induced osteoporosis, but according to Saag, many doctors are hoping Forteo is part of the "new wave" of drugs to treat the condition, and there was insufficient evidence of how it compared to the currently recommended ones. See Full Article
 The US Food and Drug Administration (FDA) has asked the manufacturer of diabetes type 2 drug Avandia (rosiglitazone maleate) to carry out a new long term study to assess the cardiovascular risk of the drug. In the meantime it will stay on the market but carry a higher level of boxed warning about potential increased risk of heart attacks, said the agency in a statement on 14th November. The FDA said doctors should monitor patients who take Avandia for any potential cardiovascular risks, and people with type 2 diabetes who are at higher risk of heart attack or who have underlying heart disease should make sure the new health warning is considered when they talk to their health care provider about available treatments. Dr. Janet Woodcock, deputy commissioner for scientific and medical programs, chief medical officer, and acting director of the Center for Drug Evaluation and Research at the FDA said the agency had: "Moved expeditiously to review the cardiovascular risks of this drug so that we could inform patients and doctors at the earliest possible time of our findings." "FDA remains committed to making sure that doctors and patients have the latest information about the risks and benefits of medicines," she added. Avandia (rosiglitazone maleate) is made by global pharmaceutical giant GlaxoSmithKline (GSK), which in the US is headquartered in Philadelphia, Pennsylvania. The drug has been prescribed to more than 7 million people over the last 7 years to help them control blood sugar. The FDA approved the drug in 1999 as an adjunct to diet and exercise, either on its own or in combination with other oral anti-diabetes drugs, metformin and sulfonylureas. Over the last 12 months the FDA has been reviewing several studies showing conflicting results about the side effects of Avandia, such as the risk of chest pain, heart attacks, deaths related to heart problems and deaths from any cause. The agency has concluded that the evidence is not sufficient to show conclusively that Avandia is any riskier than some other oral drugs for treating type 2 diabetes and has therefore asked GSK to set up a new long term study to assess the cardiovascular risks of Avandia. GSK has agreed to carry out such a study and said it will do so promptly. See Full Article
 Another outbreak of bird flu is suspected at a second farm in Suffolk, UK. The birds at Grove farm in Botesdale were scheduled to be culled following the confirmed discovery of the deadly H5N1 virus at nearby Redgrave Park farm on Tuesday. But when officials from the Department for Environment, Food and Rural Affairs (DEFRA) arrived at Grove farm to start the culling of 5,500 turkeys, they found some of the birds were already dead. Cause of death is suspected to be bird flu, thus the cull became "slaughter on suspicion". Grove farm was one of four premises identified by DEFRA as "dangerous contacts", within the restriction zone around Redgrove Park, near Diss in Norfolk, and whose poultry was destined to be culled as a precautionary measure. The other three farms where culls are taking place are: Hill Meadow in Knettishall, also in Suffolk, and two in Norfolk, Stone House Farm in West Harling, and Bridge Farm in Pulham. A total of 22,000 free range turkeys are being culled on the four farms, categorized as "dangerous contacts" because of the strong possibility that the virus may have been spread by farm workers who traveled between the farms. See Full Article
Here's a way to check your diagnostic skills.. BackgroundA 60-year-old man presents to the emergency department (ED) for pain in the right side of his chest after accidentally tripping over a sidewalk curb and falling. The patient states that when he fell he hit the right side of his chest on the sidewalk. On the review of systems, the patient does not report any shortness of breath or difficulty breathing, but he does report occasionally having a dry cough. He states that he has had the cough “for quite some time,” and he attributes it to his 40-pack-year history of smoking cigarettes. On further questioning, he denies having any weight loss, hemoptysis, or shortness of breath. On physical examination, the patient’s vital signs are noted to be normal and stable; his heart rate is 85 bpm, his blood pressure is 120/85 mm Hg, and he has an oxygen saturation of 99% while breathing room air. The patient is a man of moderate build in no apparent distress. He has normal breath sounds. The findings of the chest and abdominal examinations are unremarkable except for mild tenderness to palpation over the right chest wall; the general physical examination is otherwise unremarkable.  Chest radiographs are obtained to evaluate for possible injuries to the patient’s ribs and lungs. As a result of the radiographic findings (see Images 1-2), a complete blood count (CBC) and chemistry panel are ordered, but the results are unremarkable. The abnormality noted on the plain radiographs, combined with poor follow-up for the patient, prompts a contrast-enhanced computed tomography (CT) scan of the chest (Image 3). HintThe diagnosis is the most common benign tumor of the lung. AnswerSee Answer
Compiled and Summarized by Anthony Diabetes mellitus Diabetes mellitus (IPA: [ˌdaɪəˈbiːtiːz] or [ˌdaɪəˈbiːtəs], [məˈlaɪtəs] or [ˈmɛlətəs]), often simply diabetes (Greek: Διαβήτης), is a syndrome characterized by disordered metabolism and inappropriately high blood sugar (hyperglycemia) resulting from either low levels of the hormone insulin or from abnormal resistance to insulin's effects coupled with inadequate levels of insulin secretion to compensate. The characteristic symptoms are excessive urine production (polyuria), excessive thirst and increased fluid intake (polydipsia), and blurred vision; these symptoms are likely absent if the blood sugar is only mildly elevated. The World Health Organization recognizes three main forms of diabetes mellitus: type 1, type 2, and gestational diabetes (occurring during pregnancy), which have similar signs, symptoms, and consequences, but different causes and population distributions. While, ultimately, all forms are due to the beta cells of the pancreas being unable to produce sufficient insulin to prevent hyperglycemia, the causes are different. Type 1 diabetes is usually due to autoimmune destruction of the pancreatic beta cells, which produce insulin. Type 2 diabetes is characterized by insulin resistance in target tissues, this causes a need for abnormally high amounts of insulin and diabetes develops when the beta cells cannot meet this demand. Gestational diabetes is similar to type 2 diabetes in that it involves insulin resistance; the hormones of pregnancy can cause insulin resistance in women genetically predisposed to developing this condition. Gestational diabetes typically resolves with delivery of the child, however types 1 and 2 diabetes are chronic conditions. All types have been treatable since insulin became medically available in 1921. Type 1 diabetes, in which insulin is not secreted by the pancreas, is directly treatable only with injected or inhaled insulin, although dietary and other lifestyle adjustments are part of management. Type 2 may be managed with a combination of dietary treatment, tablets and injections and, frequently, insulin supplementation. While insulin was originally produced from natural sources such as porcine pancreas, most insulin used today is produced through genetic engineering, either as a direct copy of human insulin, or human insulin with modified molecules that provide different onset and duration of action. Insulin can also be delivered continuously by a specialized pump which subcutaneously provides insulin through a changeable catheter. Diabetes can cause many complications. Acute complications (hypoglycemia, ketoacidosis or nonketotic hyperosmolar coma) may occur if the disease is not adequately controlled. Serious long-term complications include cardiovascular disease (doubled risk), chronic renal failure, retinal damage (which can lead to blindness), nerve damage (of several kinds), and microvascular damage, which may cause impotence and poor healing. Poor healing of wounds, particularly of the feet, can lead to gangrene, which may require amputation. Adequate treatment of diabetes, as well as increased emphasis on blood pressure control and lifestyle factors (such as not smoking and keeping a healthy body weight), may improve the risk profile of most aforementioned complications. In the developed world, diabetes is the most significant cause of adult blindness in the non-elderly, the leading cause of non-traumatic amputation in adults, and diabetic nephropathy is the main illness requiring renal dialysis. Signs and SymptomsThe classical triad of diabetes symptoms is polyuria, polydipsia and polyphagia, which are, respectively, frequent urination; increased thirst and consequent increased fluid intake; and increased appetite. Symptoms may develop quite rapidly (weeks or months) in type 1 diabetes, particularly in children. However, in type 2 diabetes the symptoms develop much more slowly and may be subtle or completely absent. Type 1 diabetes may also cause weight loss (despite normal or increased eating) and irreducible fatigue. These symptoms can also manifest in type 2 diabetes in patients whose diabetes is poorly controlled. When the glucose concentration in the blood is raised beyond the renal threshold, reabsorption of glucose in the proximal renal tubuli is incomplete, and part of the glucose remains in the urine (glycosuria). This increases the osmotic pressure of the urine and inhibits the reabsorption of water by the kidney, resulting in increased urine production (polyuria) and increased fluid loss. Lost blood volume will be replaced osmotically from water held in body cells, causing dehydration and increased thirst. Prolonged high blood glucose causes glucose absorption, which leads to changes in the shape of the lenses of the eyes, resulting in vision changes. Blurred vision is a common complaint leading to a diabetes diagnosis; type 1 should always be suspected in cases of rapid vision change whereas type 2 is generally more gradual, but should still be suspected. Patients (usually with type 1 diabetes) may also present with diabetic ketoacidosis (DKA), an extreme state of metabolic dysregulation characterized by the smell of acetone on the patient's breath; a rapid, deep breathing known as Kussmaul breathing; polyuria; nausea; vomiting and abdominal pain; and any of many altered states of consciousness or arousal (such as hostility and mania or, equally, confusion and lethargy). In severe DKA, coma may follow, progressing to death. Diabetic ketoacidosis is a medical emergency and requires hospital admission. A rarer but equally severe possibility is hyperosmolar nonketotic state, which is more common in type 2 diabetes and is mainly the result of dehydration due to loss of body water. Often, the patient has been drinking extreme amounts of sugar-containing drinks, leading to a vicious circle in regard to the water loss. CauseDrugs such as steroids, Dilantin, and others may elevate the blood sugar through a variety of mechanisms. Certain other drugs, such as alloxan, streptozocin, and thiazide diuretics, are toxic to the beta cells of the pancreas and can cause diabetes. Certain syndromes (for example, Prader-Willi, Down's, Progeria, and Turner's) may result in a hyperglycemic state; if this state is prolonged, the result can be permanent diabetes. Diabetes resulting in an insulin-dependent state is classified as Type 1 diabetes. While Type 1 diabetes affects only between 5 to10 percent of the diabetic population, its effects on the body can be worse than other forms of diabetes. In the past, Type 1 has been known as juvenile or juvenile-onset diabetes (because it is usually diagnosed in those under thirty), brittle diabetes, unstable diabetes, and ketosis-prone diabetes. People in this classification more frequently exhibit the classic symptoms, usually with ketones present in blood and urine. A blood-sugar level of 800 mg/dl (44 mmol) or more, especially if ketones are not present, indicates a diagnosis of hyperglycemic hyperosmolar nonketotic syndrome (a state in which the body is extremely dry (dehydrated), the chemicals in the body are concentrated, and the blood sugar is high). As stated before, diabetes is a syndrome or group of diseases (rather than one disease), leading to the prolonged hyperglycemic state. Type 1 is most associated with the killing of the beta cells, most likely by the body's own immune system. Either the immune system cannot kill an infecting agent, which then kills the beta cells, or the immune system itself goes "wild," attacking the body's own tissue and destroying the beta cells. The cells of the islets of Langerhans are inflamed, resulting from an infectious-disease process (for example, mumps) or, more commonly, from an autoimmune (allergic to self) response. The autoimmune process results in the circulation of antibodies that may either cause or be caused by beta-cell death. If it is found that the antibodies cause beta-cell destruction (the body fighting what it now considers foreign to itself), the body's response to the Type 1 diabetes is much less severe (i.e., easier to control) with treatment. Until then, the outcome is a lack of available insulin. While the onset is said to be sudden, changes resulting in decreased insulin availability may have occurred over a longer period of time. In short, insulin-dependent diabetes mellitus is an inherited defect of the body's immune system, resulting in destruction of the insulin-producing beta cells of the pancreas. Heredity is a major cause of diabetes. If both parents have Type 2 diabetes, there is a chance that nearly all of their children will have diabetes. If both parents have Type 1 diabetes, fewer than 20 percent of their children will develop Type 1 diabetes. In identical twins, if one twin develops Type 2 diabetes, the chance is nearly 100 percent that the other twin will also develop it. In Type 1 diabetes, however, only 40 to 50 percent of the second twins will develop the disease, indicating that while inheritance is important, environmental factors (for example, too much food, too much stress, viral infection, and so forth) are also involved in the development of Type 1 diabetes. DiagnosisThe diagnosis of type 1 diabetes, and many cases of type 2, is usually prompted by recent-onset symptoms of excessive urination (polyuria) and excessive thirst (polydipsia), often accompanied by weight loss. These symptoms typically worsen over days to weeks; about a quarter of people with new type 1 diabetes have developed some degree of diabetic ketoacidosis by the time the diabetes is recognized. The diagnosis of other types of diabetes is usually made in other ways. These include ordinary health screening; detection of hyperglycemia during other medical investigations; and secondary symptoms such as vision changes or unexplainable fatigue. Diabetes is often detected when a person suffers a problem that is frequently caused by diabetes, such as a heart attack, stroke, neuropathy, poor wound healing or a foot ulcer, certain eye problems, certain fungal infections, or delivering a baby with macrosomia or hypoglycemia. Diabetes mellitus is characterized by recurrent or persistent hyperglycemia, and is diagnosed by demonstrating any one of the following: · fasting plasma glucose level at or above 126 mg/dL (7.0 mmol/l). · plasma glucose at or above 200 mg/dL (11.1 mmol/l) two hours after a 75 g oral glucose load as in a glucose tolerance test. · random plasma glucose at or above 200 mg/dL (11.1 mmol/l). A positive result, in the absence of clinical symptoms of diabetes, should be confirmed by another of the above-listed methods on a different day. Most physicians prefer to measure a fasting glucose level because of the ease of measurement and the considerable time commitment of formal glucose tolerance testing, which takes two hours to complete. According to the current definition, two fasting glucose measurements above 126 mg/dL (7.0 mmol/l) is considered diagnostic for diabetes mellitus. Patients with fasting glucose levels between 110 and 125 mg/dL (6.1 and 7.0 mmol/l) are considered to have impaired fasting glycemia. Patients with plasma glucose at or above 140 mg/dL or 7.8 mmol/l two hours after a 75 g oral glucose load are considered to have impaired glucose tolerance. Of these two pre-diabetic states, the latter in particular is a major risk factor for progression to full-blown diabetes mellitus as well as cardiovascular disease. While not used for diagnosis, an elevated level of glucose irreversibly bound to hemoglobin (termed glycosylated hemoglobin or HbA1c) of 6.0% or higher (the 2003 revised U.S. standard) is considered abnormal by most labs; HbA1c is primarily used as a treatment-tracking test reflecting average blood glucose levels over the preceding 90 days (approximately). However, some physicians may order this test at the time of diagnosis to track changes over time. The current recommended goal for HbA1c in patients with diabetes is <7.0%, which is considered good glycemic control, although some guidelines are stricter (<6.5%). People with diabetes who have HbA1c levels within this range have a significantly lower incidence of complications from diabetes, including retinopathy and diabetic nephropathy. PathogenesisFor IDDM or Type I DM, see link. For NIDDM or Type 2 DM, see link. PathophysiologyInsulin is the principal hormone that regulates uptake of glucose from the blood into most cells (primarily muscle and fat cells, but not central nervous system cells). Therefore deficiency of insulin or the insensitivity of its receptors plays a central role in all forms of diabetes mellitus. Much of the carbohydrate in food is converted within a few hours to the monosaccharide glucose, the principal carbohydrate found in blood and used by the body as fuel. Some carbohydrates are not so converted. Notable examples include fruit sugar (fructose), usable as cellular fuel but it is not converted to glucose, and which therefore does not participate in the insulin/glucose metabolic regulatory mechanism. Additionally, the carbohydrate cellulose (though it is actually many glucose molecules in long chains) is not converted to glucose, as humans and many animals have no digestive pathway capable of breaking up cellulose. Insulin is released into the blood by beta cells (β-cells), found in the Islets of Langerhans in the pancreas, in response to rising levels of blood glucose after eating. Insulin is used by about two-thirds of the body's cells to absorb glucose from the blood for use as fuel, for conversion to other needed molecules, or for storage. Insulin is also the principal control signal for conversion of glucose to glycogen for internal storage in liver and muscle cells. Lowered glucose levels result both in the reduced release of insulin from the beta cells and in the reverse conversion of glycogen to glucose when glucose levels fall. This is mainly controlled by the hormone glucagon which acts in an opposite manner to insulin. Glucose thus recovered by the liver re-enters the bloodstream; muscle cells lack the necessary export mechanism. Higher insulin levels increase many anabolic ("building up") processes such as cell growth and duplication, protein synthesis, and fat storage. Insulin (or its lack) is the principal signal in converting many of the bidirectional processes of metabolism from a catabolic to an anabolic direction, and vice versa. In particular, a low insulin level is the trigger for entering or leaving ketosis (the fat burning metabolic phase). If the amount of insulin available is insufficient, if cells respond poorly to the effects of insulin (insulin insensitivity or resistance), or if the insulin itself is defective, then glucose will not be absorbed properly by those body cells that require it nor will it be stored appropriately in the liver and muscles. The net effect is persistent high levels of blood glucose, poor protein synthesis, and other metabolic derangements, such as acidosis. PreventionType 1 diabetes risk is known to depend upon a genetic predisposition based on HLA types (particularly types DR3 and DR4), an unknown environmental trigger (suspected to an infection in most cases), and an uncontrolled autoimmune response that attacks the insulin producing beta cells. Some research has suggested that breastfeeding decreased the risk; various other nutritional risk factors are being studied, but no firm evidence has been found. Type 2 diabetes risk can be reduced in many cases by making changes in diet and increasing physical activity. The American Diabetes Association (ADA) recommends maintaining a healthy weight, getting at least 2½ hours of exercise per week (a brisk sustained walk appears sufficient), having a modest fat intake, and eating a good amount of fiber and whole grains. The ADA does not recommend alcohol consumption as a preventative, but it is interesting to note that moderate alcohol intake may reduce the risk (though heavy consumption clearly increases damage to body systems significantly). There is inadequate evidence that eating foods of low glycemic index is clinically helpful. Some studies have shown delayed progression to diabetes in predisposed patients through prophylactic use of metformin, rosiglitazone, or valsartan. In patients on hydroxychloroquine for rheumatoid arthritis, incidence of diabetes was reduced by 77%. Breastfeeding might also be correlated with the prevention of type 2 of the disease in mothers. TreatmentDiabetes mellitus is currently a chronic disease, without a cure, and medical emphasis must necessarily be on managing/avoiding possible short-term as well as long-term diabetes-related problems. There is an exceptionally important role for patient education, dietetic support, sensible exercise, self glucose monitoring, with the goal of keeping both short-term blood glucose levels, and long term levels as well, within acceptable bounds. Careful control is needed to reduce the risk of long term complications. This can be achieved with combinations of diet, exercise and weight loss (type 2), various oral diabetic drugs (type 2 only), and insulin use (type 1 and increasingly for type 2 not responding to oral medication). In addition, given the associated higher risks of cardiovascular disease, lifestyle modifications should be undertaken to control blood pressure and cholesterol by exercising more, smoking cessation, consuming an appropriate diet, wearing diabetic socks, and if necessary, taking any of several drugs to reduce pressure. In countries using a general practitioner system, such as the United Kingdom, care may take place mainly outside hospitals, with hospital-based specialist care used only in case of complications, difficult blood sugar control, or research projects. In other circumstances, general practitioners and specialists share care of a patient in a team approach. Optometrists, podiatrists/chiropodists, dietitians, physiotherapists, clinical nurse specialists (eg, Certified Diabetes Educators and DSNs (Diabetic Specialist Nurse)), or nurse practitioners may jointly provide multidisciplinary expertise. In countries where patients must provide their own health care, the impact of out-of-pocket costs of diabetic care can be high. In addition to the medications and supplies needed, patients are often advised to receive regular consultation from a physician (eg, at least every three to six months). ComplicationsPeople with diabetes may experience many serious, long-term complications. Some of these complications begin within months of the onset of diabetes, although most tend to develop after a few years. Most of the complications are progressive. The more tightly a person with diabetes is able to control the levels of sugar in the blood, the less likely it is that these complications will develop or become worse. High sugar levels cause narrowing of both the small and large blood vessels. Complex sugar-based substances build up in the walls of small blood vessels, causing them to thicken and leak. As they thicken, they supply less blood, especially to the skin and nerves. Poor control of blood sugar levels also tends to cause the levels of fatty substances in the blood to rise, resulting in atherosclerosis and decreased blood flow in the larger blood vessels. Atherosclerosis is between 2 and 6 times more common in people with diabetes than in people who do not have the disease and tends to occur at younger ages. Over time, elevated levels of sugar in the blood and poor circulation can harm the heart, brain, legs, eyes, kidneys, nerves, and skin, resulting in angina, heart failure, strokes, leg cramps on walking (claudication), poor vision, renal failure, damage to nerves (neuropathy), and skin breakdown. Heart attacks and strokes are more common among people with diabetes. Poor circulation to the skin can lead to ulcers and infections, and all wounds heal slowly. People with diabetes are particularly likely to have ulcers and infections of the feet and legs. Too often, these wounds heal slowly or not at all, and amputation of the foot or part of the leg may be needed. People with diabetes often develop bacterial and fungal infections, typically of the skin. When the levels of sugar in the blood are high, white blood cells cannot effectively fight infections. Any infection that develops tends to be more severe. Damage to the blood vessels of the eye can cause loss of vision (diabetic retinopathy. Laser surgery can seal the leaking blood vessels of the eye and prevent permanent damage to the retina. Therefore, people with diabetes should have yearly eye examinations to check for damage. The kidneys can malfunction, resulting in kidney failure that may require dialysis or kidney transplantation. Doctors usually check the urine of people with diabetes for abnormally high levels of protein (albumin), which is an early sign of kidney damage. At the earliest sign of kidney complications, the person is often given angiotensin-converting enzyme (ACE) inhibitors, drugs that slow the progression of kidney disease. Damage to nerves can manifest in several ways. If a single nerve malfunctions, an arm or leg may suddenly become weak. If the nerves to the hands, legs, and feet become damaged (diabetic polyneuropathy), sensation may become abnormal, and tingling or burning pain and weakness in the arms and legs may develop. Damage to the nerves of the skin makes repeated injuries more likely because the person cannot sense changes in pressure or temperature. Referenceshttp://www.wikipedia.orgServed as primary source. http://www.merck.comServed as secondary source and reference. http://www.gpnotebook.co.ukProvided information on Pathogenesis. http://nursing-resource.com/If you find an error, please let us know.
|

 A 55 year old nurse from Thornton Heath, Surrey was suspended on Friday, 23 November, 2007 at a Conduct and Competence hearing of the Nursing and Midwifery Council in London.
A 55 year old nurse from Thornton Heath, Surrey was suspended on Friday, 23 November, 2007 at a Conduct and Competence hearing of the Nursing and Midwifery Council in London. New research funded by the MS Society has shown that Botox injections to the bladder provide benefits for people with multiple sclerosis (MS) with sustained improvements to their overall quality of life.
New research funded by the MS Society has shown that Botox injections to the bladder provide benefits for people with multiple sclerosis (MS) with sustained improvements to their overall quality of life.
 A breakthrough in stem cell research was announced last week in a paper in the journal Science where researchers from the University of Wisconsin -Madison in the US and other colleagues reported how they reprogrammed human skin cells to behave like embryonic stem cells.
A breakthrough in stem cell research was announced last week in a paper in the journal Science where researchers from the University of Wisconsin -Madison in the US and other colleagues reported how they reprogrammed human skin cells to behave like embryonic stem cells. Normal Spontaneous Vaginal Delivery a.k.a. Vaginal Birth, Spontaneous Vaginal Delivery, Normal Vaginal Delivery, is the term used to describe any delivery of the baby through the vagina (versus a c-section delivery). The baby typically comes through head first. If the baby is not head first, (e.g., breech) it may need to be delivered by
Normal Spontaneous Vaginal Delivery a.k.a. Vaginal Birth, Spontaneous Vaginal Delivery, Normal Vaginal Delivery, is the term used to describe any delivery of the baby through the vagina (versus a c-section delivery). The baby typically comes through head first. If the baby is not head first, (e.g., breech) it may need to be delivered by 
 An X-ray machine utilizes electromagnetic radiation to produce an image of an object, usually with the purpose of visualizing something located below the object's surface. The machine is made up of an X-ray source or X-ray tube, an x-ray detection system, and positioning hardware to align these two components with the object to be imaged.
An X-ray machine utilizes electromagnetic radiation to produce an image of an object, usually with the purpose of visualizing something located below the object's surface. The machine is made up of an X-ray source or X-ray tube, an x-ray detection system, and positioning hardware to align these two components with the object to be imaged. X-rays (or Röntgen rays) are a form of electromagnetic radiation with a wavelength in the range of 10 to 0.01 nanometers, corresponding to frequencies in the range 30 PHz to 30 EHz. X-rays are primarily used for diagnostic radiography and crystallography. X-rays are a form of ionizing radiation and as such can be dangerous. In many languages it is called Röntgen radiation after one of the first investigators of the X-rays, Wilhelm Conrad Röntgen.
X-rays (or Röntgen rays) are a form of electromagnetic radiation with a wavelength in the range of 10 to 0.01 nanometers, corresponding to frequencies in the range 30 PHz to 30 EHz. X-rays are primarily used for diagnostic radiography and crystallography. X-rays are a form of ionizing radiation and as such can be dangerous. In many languages it is called Röntgen radiation after one of the first investigators of the X-rays, Wilhelm Conrad Röntgen. A new US study suggests that the osteoporosis drug Forteo (made by Eli Lilly) was more effective than Fosamax (made by Merck) at increasing bone density in arthritis patients with osteoporosis caused by taking corticosteroids such as prednisone.
A new US study suggests that the osteoporosis drug Forteo (made by Eli Lilly) was more effective than Fosamax (made by Merck) at increasing bone density in arthritis patients with osteoporosis caused by taking corticosteroids such as prednisone. The US Food and Drug Administration (FDA) has asked the manufacturer of diabetes type 2 drug Avandia (rosiglitazone maleate) to carry out a new long term study to assess the cardiovascular risk of the drug. In the meantime it will stay on the market but carry a higher level of boxed warning about potential increased risk of heart attacks, said the agency in a statement on 14th November.
The US Food and Drug Administration (FDA) has asked the manufacturer of diabetes type 2 drug Avandia (rosiglitazone maleate) to carry out a new long term study to assess the cardiovascular risk of the drug. In the meantime it will stay on the market but carry a higher level of boxed warning about potential increased risk of heart attacks, said the agency in a statement on 14th November. Another outbreak of bird flu is suspected at a second farm in Suffolk, UK. The birds at Grove farm in Botesdale were scheduled to be culled following the confirmed discovery of the deadly H5N1 virus at nearby Redgrave Park farm on Tuesday.
Another outbreak of bird flu is suspected at a second farm in Suffolk, UK. The birds at Grove farm in Botesdale were scheduled to be culled following the confirmed discovery of the deadly H5N1 virus at nearby Redgrave Park farm on Tuesday.